Elizabeth Jones
Survivor
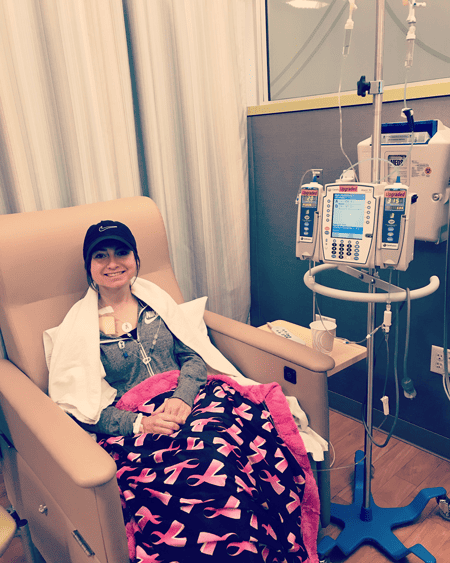
Being so young, still at the beginning of my career as a registered nurse, focusing on ways to better myself for my patients, the last thing on my mind was thinking I had cancer, but that quickly changed. On March 29th, 2019 I received the news that no 25-year-old wanted to hear, “You have invasive breast cancer.” I was completely shocked and devastated by the news. With this shocking news, I knew it was time for a change to not only focus on my patient’s life but focusing on ways to make mine healthier. During my monthly self-breast exam I had felt something that did not seem normal to me. While I was in for my yearly check up with my OBGYN, I mentioned my finding to her. She seemed to think that it was just benign fibroadenoma that most women my age have, but she went ahead and ordered an ultrasound to be safe. During the ultrasound, they found three solid masses and recommended a mammogram to be performed. I completed the mammogram, but the scans were not clear as I was noted to have dense breast tissue, as most younger women have. At this point, they recommended a core needle biopsy to figure out what was going on inside my breast. Throughout my testing I was constantly reassured by multiple doctors and nurses, “You are so young, this is probably just benign, you will be just fine.” But, I have come to learn breast cancer is quite common and that one in eight women are diagnosed with breast cancer in their life. On March 29th, 2019 my life changed when I received the phone call from my doctor hearing that my breast biopsy results came back positive for invasive ductal/mammary carcinoma (IDC). I soon learned that my cancer was ER/PR + (estrogen/progesterone positive), which was some good news, as I was told by my doctor anyways. She informed me that breast cancers that are typically found in my age are aggressive and fast growing, but the type I have been diagnosed with was the type that is seen more with older women and is slower growing and that it was estrogen/progesterone responsive, meaning that after surgical/medical treatment, I will respond well to an estrogen-blocking medication. The doctors took weeks running all kinds of test and going over my family history trying to figure out why a 25-year-old has breast cancer that is typically seen later in a person’s life. I had no immediate family history of breast cancer. Thankfully, one of the tests gave them the answers they were looking for. I was found to have a genetic mutation known as CHEK 2, which put me at high risk for breast cancer as well as other cancers. I met with multiple wonderful doctors including a surgical oncologist, medical oncologist, plastic surgeon, and fertility specialist to develop my treatment plan. My surgical plan included a double mastectomy. I chose a double mastectomy because of the genetic mutation I have, which has a high percentage of my breast cancer coming back in my other breast. After that, I began the process of undergoing IVF egg retrieval with a fertility specialist due to chemotherapy and the estrogen-blocking medication increasing my risk of infertility. Once I completed the egg retrieval process, my medical treatment began. This included 4 rounds of chemotherapy. After chemotherapy I was on my final treatment regimen, Zoladex & Anastrozole, estrogen-blocking medications that I will take for 10 years to prevent reoccurrence.
