What is lymphedema?
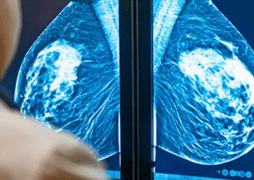
Lymph is a clear fluid that contains white blood cells (these cells help fight infections). Lymph vessels, like blood vessels, run all through the body carrying lymph, cells and other material. Lymph from tissues and organs drains into the lymph vessels and is carried to the lymph nodes where it is filtered. While lymph nodes are found throughout the body, the ones near the breast (see image below) are those affected during treatment for breast cancer.
Image source: National Cancer Institute (http://www.cancer.gov)
During surgery (mastectomy or lumpectomy) for breast cancer, some of the lymph nodes in the underarm (called axillary lymph nodes) are removed and checked to see if the cancer has spread to these lymph nodes. When axillary lymph nodes are removed during breast surgery (or are affected by radiation therapy), some of the vessels that carry lymph fluid can become blocked. This may prevent lymph fluid from leaving the area.
Lymphedema occurs when lymph fluid collects in the arm (or other area such as the hand, fingers, chest or back) and causes swelling (edema). This swelling may be so slight it is barely noticed or it may be so great the arm grows large. In severe cases, lymphedema can cause pain and limit movement.
Who gets lymphedema?
Lymphedema is related to breast surgery and radiation therapy, but it is not clear why some breast cancer survivors get lymphedema and others do not. However, a few factors increase risk, including:1-4
- Removal of a large number of axillary lymph nodes (axillary lymph node surgery) during breast cancer surgery
- Radiation to the axillary lymph nodes
- A combination of axillary lymph node surgery and radiation to the axillary lymph nodes
- Having a large number of axillary lymph nodes that contain cancer
- Infections in the area after surgery
- Being overweight
When does lymphedema occur?
Lymphedema usually occurs within three years of breast surgery.2 Sometimes it occurs immediately after surgery and sometimes it can take many years to develop.
How often does lymphedema occur?
The good news is that most breast cancer survivors don’t get lymphedema. And, because modern surgery removes fewer lymph nodes, lymphedema has become less common and the cases that do occur are less severe.
In the past, most people had a procedure called axillary dissection to remove axillary lymph nodes. Now, most people have a sentinel node biopsy (SNB), which removes fewer lymph nodes than axillary dissection and thus, lowers the risk of lymphedema.1-9 A recent study found that 10 years after breast surgery, only about five percent of survivors who had SNB had developed lymphedema versus about 35 percent of those who had axillary dissection.9
Does breast reconstruction impact lymphedema?
For women who choose breast reconstruction after a mastectomy, the type of reconstruction does not appear to affect the risk of lymphedema.4
What are the symptoms of lymphedema?
Breast cancer survivors who have symptoms of lymphedema should see their health care provider if they notice any of the following:
| Symptoms of lymphedema1-2 |
| Swelling in the arm or hand (for example, you may notice a tighter fit of rings or watches)Feeling of tightness, heaviness or fullness in the arm or handFeeling of tightness in the skin or a thickening of the skinPain or redness in the arm or hand |
Are there standard methods of screening and diagnosis of lymphedema?
There are no standard screening tools for lymphedema and there is no standard way to diagnose lymphedema.
The most common way for providers to check for lymphedema is by measuring upper and lower arm widths. These measurements may be taken before surgery to have a comparison for measures taken after surgery. Other screening methods include water displacement, perometers, photography, bioimpedance measures and special imaging called lymphoscintigraphy (only available at some medical centers).2,10-15
How is lymphedema treated?
Although there is no cure for lymphedema, treatment can improve movement and reduce pain and swelling in the affected arm. Standard lymphedema treatment includes complex decongestive therapy. The goal of this therapy is to decrease swelling and infection related to lymphedema through a combination of: 1,14-19
- Skin and nail care
- Compression bandages or sleeves (these apply pressure around the arm and help push lymph fluid out of the arm)
- Exercises (closing and opening a fist, for example)
- Manual lymphatic drainage (a special type of massage)
- Physical therapy
Other treatments include exercise, weight loss, surgery and use of a compression device (a pump connected to a sleeve that inflates and deflates to apply pressure to the arm).1,14-15,19-20 New treatments for lymphedema, such as laser therapy, are under study.15
Does exercise cause lymphedema?
In the past, there was some concern that exercise might increase the risk of lymphedema in breast cancer survivors and worsen symptoms in those who developed the condition.
Strenuous exercise should be avoided immediately after breast surgery. However, after recovery, arm exercises (such as weight-lifting) do not appear to increase the risk of lymphedema.19,21-23 And, for those who develop lymphedema, studies now show weight-lifting (in a supervised setting) can reduce symptoms and improve body image, sexuality and physical strength.19,22-24
Can lymphedema be prevented?
There is no proven way to prevent lymphedema. However, injury or infection to the arm may trigger it,6 so taking steps to reduce these risks may be helpful for some people. It is important to note the tips listed below have not been proven in clinical trials.
| Tips on reducing the risk of injury or infection to the arm2,25 |
| Treat infections of the at-risk arm and hand right away.Wear gloves when doing house or garden work.Keep skin clean and well-moisturized.Use the arm not at risk when having blood drawn, getting injections or having blood pressure taken.Avoid sunburn and excess heat from saunas, hot baths, tanning and other sources.Do not cut nail cuticles.Use insect repellant when outdoors.Avoid injuries, including scratches and bruises, to the at-risk arm.Rest the at-risk arm in an elevated position (above the heart or shoulder). |
Summary
Lymphedema occurs less often today than in the past thanks to the increased use of sentinel node biopsy. According to Dr. Terry Mamounas, Director, Comprehensive Breast Center, MD Anderson Cancer Center, Orlando, “the adoption and widespread use of sentinel lymph node biopsy over axillary lymph node dissection has resulted in a dramatic decrease in the risk for lymphedema over the past several years.
Further improvements in our understanding of lymphedema risk factors and newer management approaches provide patients with additional options for lymphedema prevention and management.
We are optimistic that in the years to come the incidence of lymphedema among breast cancer survivors will continue to decline as surgical and radiation therapy interventions will be further minimized. Some of the factors contributing to this trend will include the increasing use of neoadjuvant (preoperative) chemotherapy, improvements in patient selection with novel biomarkers and continuing refinements in surgical and radiation therapy techniques.”
Although there is no proven way to prevent lymphedema, survivors can:
- Be aware that lymphedema is a possible side effect of treatment.
- Take steps to try to reduce the risk of injury and infection.
- Seek care at the first sign of symptoms.
And although there is no cure for lymphedema, when it is caught early, treatment can reduce some symptoms and stop them from getting worse. If you are a breast cancer survivor and have concerns about lymphedema, talk to your provider.
Lymphedema resources |
| Living Beyond Breast Cancer Find information on lymphedema. http://www.lbbc.org/ Lymphatic Research Foundation Find information on lymphedema and clinical trials on lymphedema. http://www.lymphaticresearch.org Lymphology Association of North America (LANA) Find a list of physical therapists. http://www.clt-lana.org National Cancer Institute—Lymphedema Find information on lymphedema. http://www.cancer.gov National Lymphedema Network Find a support group, physical therapist, financial assistance for garments and information on lymphedema. http://www.lymphnet.org CancerCare’s Linking A.R.M.S.TM Financial assistance for lymphedema supplies. http://www.cancercare.org/ |
What is Komen Doing?
Through a partnership between CancerCare and Susan G. Komen for the Cure®, Linking A.R.M.S.™ (http://www.cancercare.org/) provides financial assistance for lymphedema supplies and other breast cancer treatment-related needs. Last year, Komen awarded $500,000 to this program.
Also, Susan G. Komen’s Research, Evaluation & Scientific Programs have provided more than $2.6 million in funding for research grants studying various aspects of lymphedema. Examples of Komen-supported research include:
- Uncovering the basic biological mechanisms that lead to lymphedema
- Testing an exercise-based intervention for prevention of lymphedema in breast cancer survivors that received axillary lymph node dissection
- Developing an ultrasound device that can detect mild lymphedema in breast cancer survivors to enable early treatment Identifying and assessing new drugs that can improve or reverse the effects of lymphedema
- Testing integrative and complementary therapies that may help lymphedema
- Developing culturally appropriate and reader friendly educational materials on lymphedema for a variety of audiences
References
- McLaughlin SA, Cohen S, Van Zee KJ. Chapter 45: Lymphedema, in Harris JR, Lippman ME, Morrow M, Osborne CK. Diseases of the Breast, 4th edition. Lippincott Williams and Wilkins, 2010.
- National Cancer Institute. General information about lymphedema. http://www.cancer.gov/cancertopics/pdq/supportivecare/lymphedema/Patient, 2011.
- Ahmed RL, Schmitz KH, Prizment AE, Folsom AR. Risk factors for lymphedema in breast cancer survivors, the Iowa Women’s Health Study. Breast Cancer Res Treat. 130(3):981-91, 2011.
- Crosby MA, Card A, Liu J, Lindstrom WA, Chang DW. Immediate breast reconstruction and lymphedema incidence. Plast Reconstr Surg. 129(5):789e-95e, 2012.
- Mansel RE, Fallowfield L, Kissin M, et al. Randomized multicenter trial of sentinel node biopsy versus standard axillary treatment in operable breast cancer: the ALMANAC Trial. J Natl Cancer Inst. 98(9):599-609, 2006.
- McLaughlin SA, Wright MJ, Morris KT, et al. Prevalence of lymphedema in women with breast cancer 5 years after sentinel lymph node biopsy or axillary dissection: objective measurements. J Clin Oncol. 26(32):5213-9, 2008.
- Tsai RJ, Dennis LK, Lynch CF, Snetselaar LG, Zamba GK, Scott-Conner C. The risk of developing arm lymphedema among breast cancer survivors: a meta-analysis of treatment factors. Ann Surg Oncol. 16(7):1959-72, 2009.
- Norman SA, Localio AR, Kallan MJ, et al. Risk factors for lymphedema after breast cancer treatment. Cancer Epidemiol Biomarkers Prev. 19(11):2734-46, 2010.
- Wernicke AG, Goodman RL, Turner BC, et al. A 10-year follow-up of treatment outcomes in patients with early stage breast cancer and clinically negative axillary nodes treated with tangential breast irradiation following sentinel lymph node dissection or axillary clearance. Breast Cancer Res Treat. 125(3):893-902, 2011.
- Hayes S, Cornish B, Newman B. Comparison of methods to diagnose lymphoedema among breast cancer survivors: 6-month follow-up. Breast Cancer Res Treat. 89(3):221-6, 2005.
- Deltombe T, Jamart J, Recloux S, et al. Reliability and limits of agreement of circumferential, water displacement, and optoelectronic volumetry in the measurement of upper limb lymphedema. Lymphology. 40(1):26-34, 2007.
- Hayes S, Cornish B, Newman B. Hayes SC, Janda M, Cornish B, Battistutta D, Newman B. Lymphedema after breast cancer: incidence, risk factors, and effect on upper body function. J Clin Oncol. 26(21):3536-42, 2008.
- Stout Gergich NL, Pfalzer LA, McGarvey C, Springer B, Gerber LH, Soballe P. Preoperative assessment enables the early diagnosis and successful treatment of lymphedema. Cancer.112(12):2809-19, 2008.
- Shah C, Vicini FA. Breast cancer-related arm lymphedema: incidence rates, diagnostic techniques, optimal management and risk reduction strategies. Int J Radiat Oncol Biol Phys. 81(4):907-14, 2011.
- Paskett ED, Dean JA, Oliveri JM, Harrop JP. Cancer-related lymphedema risk factors, diagnosis, treatment, and impact: a review. J Clin Oncol. 30(30):3726-33, 2012.
- Koul R, Dufan T, Russell C, et al. Efficacy of complete decongestive therapy and manual lymphatic drainage on treatment-related lymphedema in breast cancer. Int J Radiat Oncol Biol Phys. 67(3):841-6, 2007.
- Hamner JB, Fleming MD. Lymphedema therapy reduces the volume of edema and pain in patients with breast cancer. Ann Surg Oncol. 14(6):1904-8, 2007.
- Vignes S, Porcher R, Arrault M, Dupuy A. Long-term management of breast cancer-related lymphedema after intensive decongestive physiotherapy. Breast Cancer Res Treat. 101(3):285-90, 2007.
- Hayes SC, Johansson K, Stout NL, et al. Upper-body morbidity after breast cancer: incidence and evidence for evaluation, prevention, and management within a prospective surveillance model of care. Cancer. 118(8 Suppl):2237-49, 2012.
- Saaristo AM, Niemi TS, Viitanen TP, Tervala TV, Hartiala P, Suominen EA. Microvascular breast reconstruction and lymph node transfer for postmastectomy lymphedema patients. Ann Surg. 255(3):468-73, 2012.
- McNeely ML, Campbell K, Ospina M, et al. Exercise interventions for upper-limb dysfunction due to breast cancer treatment. Cochrane Database Syst Rev. (6):CD005211, 2010.
- Schmitz KH, Ahmed RL, Troxel AB, et al. Weight lifting for women at risk for breast cancer-related lymphedema: a randomized trial. JAMA. 304(24):2699-705, 2010.
- Kwan ML, Cohn JC, Armer JM, Stewart BR, Cormier JN. Exercise in patients with lymphedema: a systematic review of the contemporary literature. J Cancer Surviv. 5(4):320-36, 2011.
- Speck RM, Gross CR, Hormes JM, et al. Changes in the Body Image and Relationship Scale following a one-year strength training trial for breast cancer survivors with or at risk for lymphedema. Breast Cancer Res Treat. 121(2):421-30, 2010.
- Showalter SL, Brown JC, Cheville AL, Fisher CS, Sataloff D, Schmitz KH. Lifestyle risk factors associated with arm swelling among women with breast cancer. Ann Surg Oncol. 2012 Oct 3. [Epub ahead of print].