Breast cancer patients from coast-to-coast struggle to access high-quality care and afford their care following a breast cancer diagnosis. But even before that diagnosis, too many people struggle to get an annual mammogram, and if that mammogram reveals an abnormal finding, they cannot afford the out-of-pocket costs for necessary follow-up testing.
Despite major public policy wins in state legislatures and in Congress during the 2021-2022 sessions, there remain inequities in health care, in the way patients are treated and in breast cancer outcomes for Black women and white women.
One way to make health care more accessible and affordable, and improve outcomes for all patients, is through changes in public policy. Susan G. Komen has identified three areas where it will work in the 2023 and 2024 state and federal legislative sessions to enact laws so that where you live does not determine if you live, and so the most vulnerable populations can get and afford the care they need to save their lives.
The three areas include accelerating research, ensuring access and alleviating patient burden, and were selected with the input of breast cancer survivors and Komen public policy advocates who believe these are three primary areas where significant, long-term changes can be made.
Accelerating research
- Additional funding for biomedical research at the state and federal level will help us discover new and more effective treatments for breast cancer so that we can save more lives. That’s because groundbreaking research is conducted at the National Institutes of Health (NIH), the Department of Defense (DOD) and through state agencies, and more funding for the agencies’ biomedical research will lead to more and better treatment options.
- Not all populations are represented in clinical trials, likely because trials are not offered to patients in an inclusive and equitable way. Educating patients about clinical research options, breaking down barriers to trial participation, and inviting them to participate would help include people from all ages, genders and ethnicities and further our ability to develop therapies that are effective in all populations. To make it possible for more diverse populations to participate, policies must require coverage of indirect costs to patients to facilitate participation (e.g., transportation, childcare, clinical navigation)
Ensuring access
- The Centers for Disease Control and Prevention’s (CDC) National Breast and Cervical Cancer Early Detection Program (NBCCEDP) provides breast cancer screening and diagnostic services for uninsured and underinsured women and has been effective at catching breast cancers early. Additional federal and state funding and expanded eligibility for these programs would allow more people to get screened and help detect breast cancers early, when treatment options and survival rates are the best.
- Medicaid provides critical services for patients who have been diagnosed with breast cancer. However, burdensome restrictions and requirements can often prevent qualifying people from accessing the services they need – therefore continued access to these programs is critical. Komen supports expanded coverage and services without impediments for enrollees (e.g., funding, work requirements, premiums, restricted eligibility).
- Currently a person diagnosed with metastatic breast cancer (MBC) – the latest stage of breast cancer for which there is currently no cure – must wait a combined 29 months to receive federal help. Komen supports removing the five-month waiting period for a person to receive Social Security Disability Insurance (SSDI) and the 24-month waiting period to receive Medicare benefits.
Alleviating patient burden
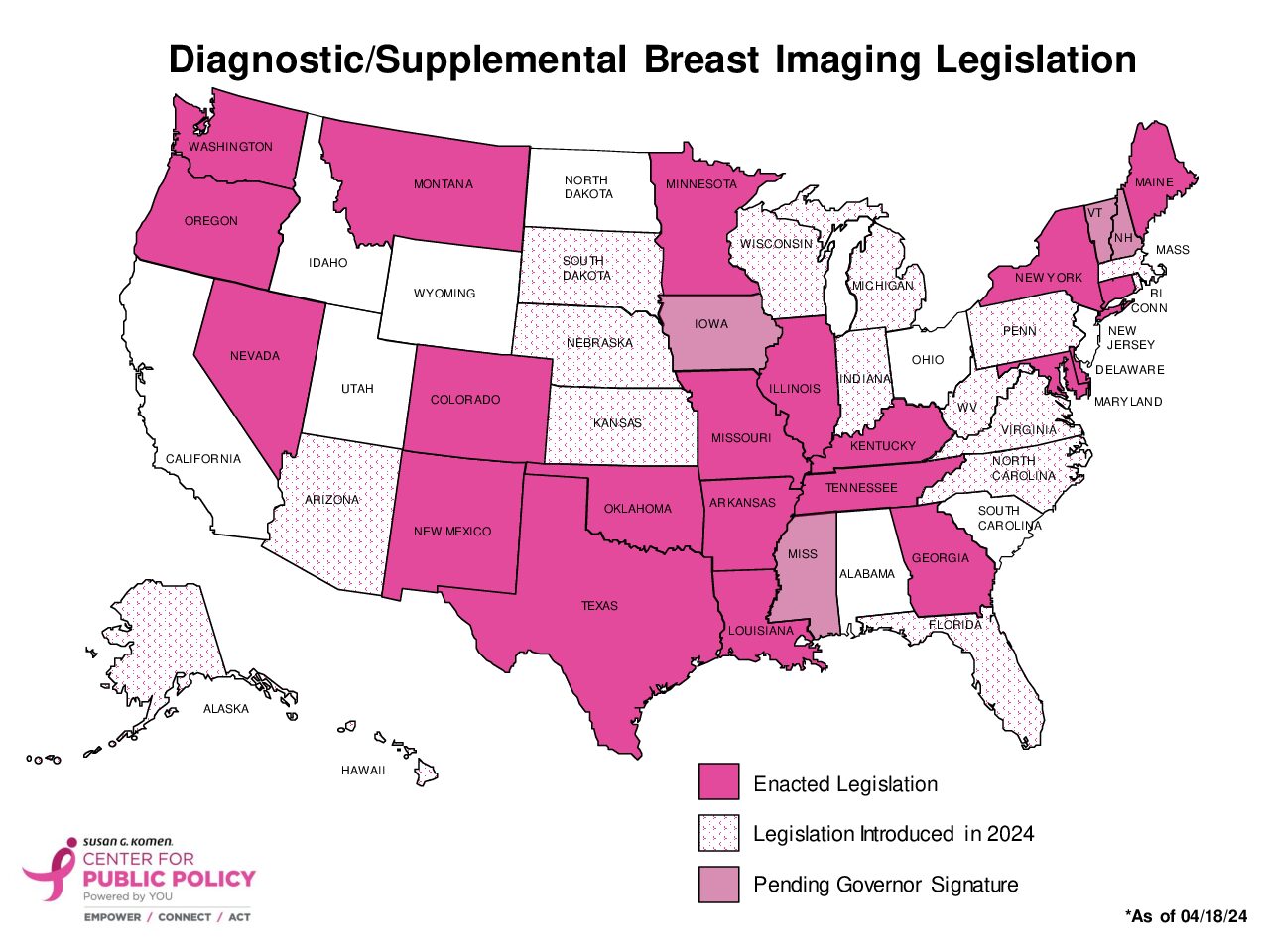
- Current law requires insurance companies to cover the cost of annual mammograms for women over the age of 40, without any cost to the woman. Unfortunately, individuals at a higher risk of breast cancer or those requiring follow-up imaging (e.g., diagnostic mammography, breast ultrasound, breast MRI) due to an abnormal mammogram result will likely be facing hundreds to thousands of dollars in patient cost sharing. Komen strongly supports policies that eliminate the out-of-pocket cost of these medically necessary tests.
- Komen supports policies that improve accessibility and affordability of genetic counseling, genetic testing and genomic testing, so a person can fully understand their risk of developing breast cancer or to help guide treatment decisions.
- Patient navigation services help a patient through the continuum of care, so they don’t get lost in a web of doctor visits, appointments and tests throughout their diagnosis and treatment. Komen supports an increase in coverage for these patient navigation services, reimbursement for the cost of the services and policies that make navigation accessible to more people.
- Remove insurance barriers related to the treatment of cancer so that patients can receive the right treatment without burdensome processes and cost. These barriers include step therapy/metastatic step therapy protocols that require a preferred drug to fail a patient before they can access the originally prescribed drug. They also include out-of-pocket costs; prior authorization requirements; co-pay accumulators, which prevent a patient from applying a drug manufacturer’s assistance coupon toward their annual out-of-pocket maximums; and non-medical switching, in which an insurance company will switch a patient’s medication for reasons unrelated to health and more commonly related to cost.